Policy. Analysis. Advocacy
Scaling Agroecology
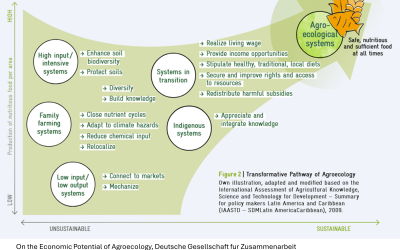
Challenges in scaling agroecology and practical pathways forward Rebecca Laes-Kushner and Harriet Keturah Traditional agriculture has brought about huge increases in food availability in the past century. But it also relies on pesticides and herbicides, focuses on...
How pooled funding and participatory grantmaking strengthen ecosystems
by Rebecca Laes-Kushner and Roy CórdovaAll too often, NGOs work in bubbles, unaware of similar or complementary work happening nearby . Donors fall into similar silos, funding projects in isolation rather than collaborating with peers who fund similar services in...
MSD Strengths and Weaknesses
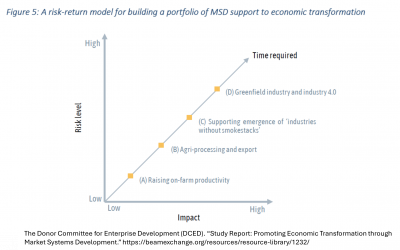
Part one of this series reviewed the main concepts behind MSD and how the approach functions. Market systems development (#MSD) is a powerful way to stimulate changes in the marketplace – by improving how goods and services are bought and sold and stimulating support...
Introduction to a Market Systems Development (MSD) Approach
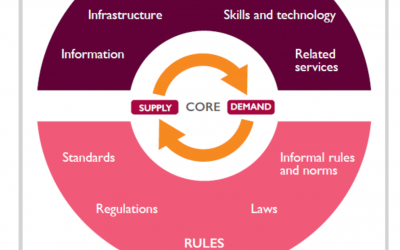
How do you raise people out of poverty? How do you improve economic conditions in a low-income region or country? Private sector development (#PSD) has been a long-standing answer. Donors support micro, small and medium enterprises (#MSMEs) by providing training in...
The strength of refugees
From trauma to limited access to education and jobs, refugees face challenges – but also show resilience, adaptability and a desire to improve their circumstances. There are over 36 million refugees worldwide, as well as approximately 70 million more people internally...
The economic and health costs of lead exposure
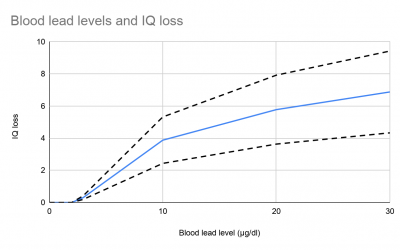
Children's exposure to lead causes 1.5 million deaths every year as well as health impacts, including lower IQs and behavioral problems, which ultimately impact adults' ability to earn sufficient wages. Lead exposure is tied to US$1.4 trillion in income loss...
Modern slavery – a global problem
Approximately 50 million people today are in slavery, including 12 million children and 22 million people in forced marriages (many of whom are children). Overview of modern slavery Although the top 10 countries are North Korea, Eritrea, Mauritania, Saudi Arabia,...
Learning Poverty
Poverty - i.e., financial poverty - is exacerbated by other poverties. Food poverty, including hunger and malnutrition, lead to health problems that impact a person's potential earnings. Similarly, inadequate schooling hinders a person's ability to find work and earn...
Small-scale farmers
The importance of small farmersMicro, small and medium enterprises (MSMEs) play a critical role in the food system in developing countries. Worldwide, SME farms produce approximately 50% of calories, over 85% of fruits and vegetables and about 80% of meat and...
Mining: Bolivia’s environmental disaster
However, higher temperatures and fires are not what worries me the most. More severe damage to the environment, with long-term impacts, has been carried out for a long time now.
I am talking about the mining sector in Bolivia. This sector processes the minerals with very basic procedures and - in the case of gold – with great amounts of mercury, dumping mineral waste into rivers, contaminating the water, fish and all biodiversity in the river banks. Families downriver cannot eat the fish anymore and they even have high mercury levels in their bodies.
Digital tools for Monitoring & Evaluation
Data collection for development projects In rural areas far from internet service or in cities with electricity or internet access disrupted by violence or shortages, some #development projects still use paper and pen forms to collect information - primary stakeholder...
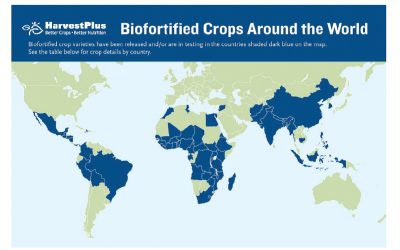
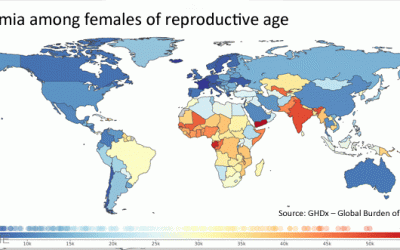
How to increase large-scale food fortification (LSFF)
Lack of micronutrients causes diseases ranging from anemia to stunting in children as well as child mortality and cognitive deficiencies. One key intervention is large-scale food fortification (#LSFF), which adds #micronutrients to food staples such as rice, wheat and...